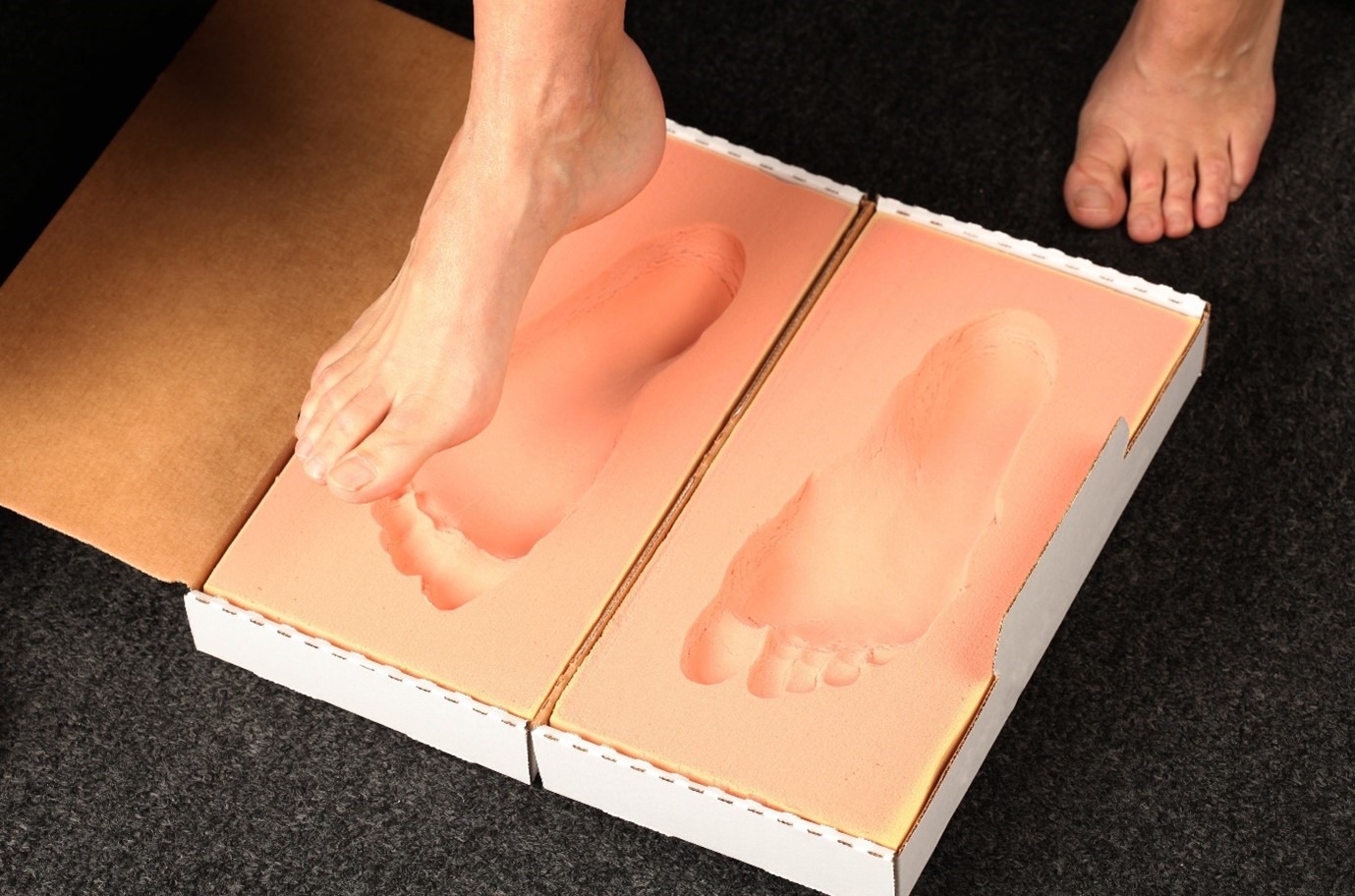
Diabetes and foot disease
Foot Orthoses for Diabetes- Diabetes is a chronic health condition where the body cannot maintain healthy levels of glucose in the blood. This may be caused by either an inability of the body to produce insulin (the hormone which processes glucose within the body) or by the body being unable to use insulin effectively. Unhealthy levels of glucose in the blood can lead to many short and long term complications including vascular complications, heart disease, kidney failure, blindness and nerve damage.
Diabetic foot disease is a leading cause of hospitalisation, amputation and disability internationally. Those with diabetes may unknowingly develop minor cuts, blisters or pressure sores due to lack of sensation. People with diabetes often have poor circulation and peripheral neuropathy which impair the body’s protective mechanisms after injury. This often results in poor wound healing, and if left untreated, complications may lead to ulceration and possible amputations.
Foot Orthotics for management of diabetic feet/ diabetes-related foot disease
Diabetic foot ulceration is the leading cause of lower limb amputation in Australia. Prevention and early treatment of ulceration is essential. Data indicates those who require amputation for management of ulceration have a 50% chance of re-amputation in the remaining limb.
Custom-made pressure-relieving foot orthoses are evidence-based interventions that can prevent diabetic foot ulcers and promote healing and protection of the feet. Custom foot orthoses are shoe inserts made specifically to reduce pressure in areas of breakdown risk, support healing of minor ulcers, and allow users to increase their levels of activity. This is achieved by supporting any structural deformities or gait abnormalities, increasing shock absorption during standing and walking, and relieving high-risk areas of pressure.
There are a number of ways in which foot orthoses reduce pressures within a foot. Firstly, we are able to redistribute areas of high pressure to areas of the foot that are more tolerable to pressure. Custom contouring/shaping of the device ensures that areas of the foot that are subject to increased pressure and ulceration are effectively offloaded and protected. Secondly, using soft foams spreads pressures over a greater surface area of the skin, resulting in a more comfortable standing and walking.

How does an Orthotist do this?
There are a number of things that must be considered when fitting custom foot orthoses. Your orthotist will assess your foot history (including callouses, previous ulcers, foot deformity or amputations) as well as your daily activities and type of footwear worn. Your orthotist will also undertake a physical assessment of your feet including walking pattern, foot posture, range of motion and strength testing of muscles around your ankle joint. This in-depth assessment ensures that your foot orthoses are tailored to your specific presentation and requirements.
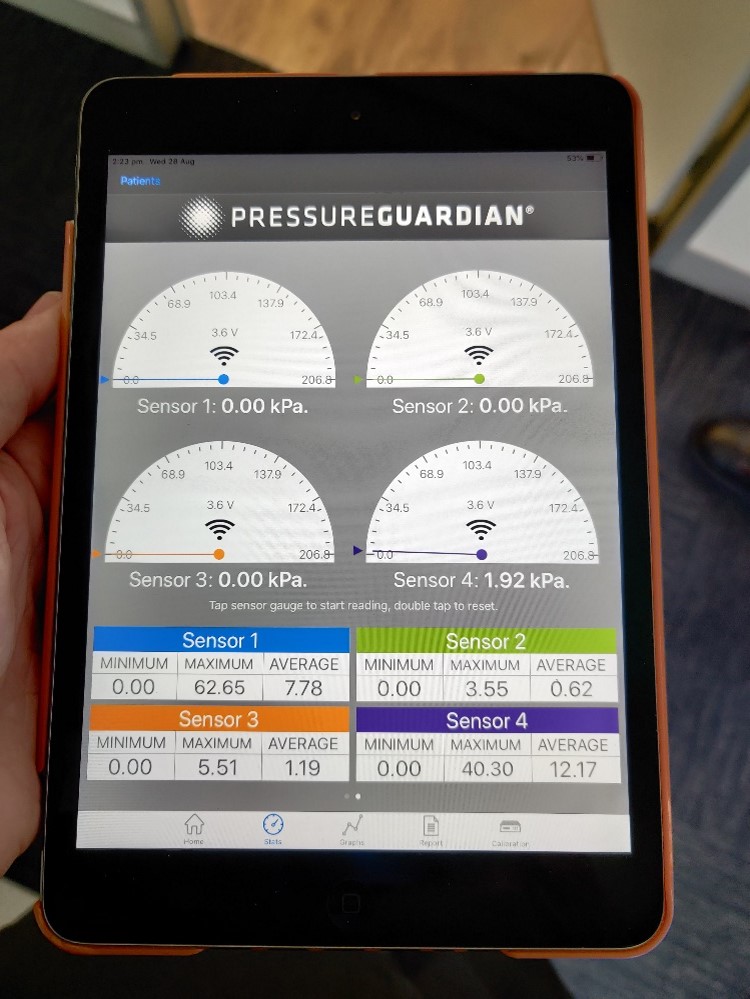
Pressure mapping
At Momentum, we use a pressure sensing tool which allows us to detect and assess areas of high pressure on the feet. This is extremely beneficial as it enables us to map and document the pressure applied to risk areas or areas of the feet where ulceration has previously occurred. This scientific assessment allows precise fine tuning of your foot orthoses to ensure appropriate offloading during standing and walking.
When undertaking any form of orthotic intervention to manage diabetic-related foot disease, it is important to continue working with your Podiatrist as they can assist you with caring for your feet, wound cleaning and dressings where necessary. Your podiatrist will aid you in monitoring your feet for changes in pressure, and devise a plan to manage your feet long term.
If you have any further questions, please feel free to contact the author.
Foot Orthoses for Diabetes? – Author: Sarah Ivey, Orthotist Prothetist
Meanwhile, anyone can reach out to staff members at (02) 6210 0060 to ask questions or schedule an in-person appointment.