A chronic condition found commonly among sports people and recreational athletes is Achilles Tendinopathy. Past treatment options are often limited due to a poor understanding of its cause. In recent years research has provided further options for treatment and that this type of injury may not involve inflammation. It is more likely caused by a series of micro tears that weaken the tendon.
Anatomy
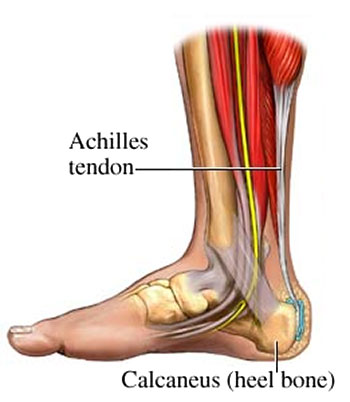
The largest tendon in the body is the Achilles Tendon and it can be found at the back of the ankle. The Achilles tendon attaches the calf muscle to the back of the heel. It is an extension of the gastrocnemius and soleus muscles. This tendon gives you the ability to push off during walking and running.
A complete or a partial tear of the Achilles tendon is known as a rupture, this occurs when the tendon is stretched beyond its capacity.
Risk
The term Achilles Tendinopathy is now used to describe Achilles tendon injuries including tendonitis. It is a common injury that many sports people suffer from especially those who are running and jumping. It is the repetitive action of stretching and potentially overstretching this tendon that leads to tendon injuries.
Injuries can occur suddenly or happen gradually over time due to ageing or repetitive tearing of the tendon. There are a number of causes that can result in Achilles tendinopathy. Forceful jumping or pivoting, sudden increases to speed when running, overstretching and even tripping or falling can result in an injury to the Achilles tendon.
Other risks include:
- Sudden increase of intensity, frequency or duration of an activity
- Not enough recovery time between activity
- Non Supportive footwear
- Uneven or hard training surfaces
- Lack of muscle flexibility
- Overtraining or excessive training
- Inadequate warm up and stretching before and after exercise
- Middle- aged people participating in sports
- Men are more likely to suffer than women
- Illness, medications and antibiotics are less common risks
Prevention
It is not always easy to prevent an injury such as Achilles tendinopathy, there are measures you can take to reduce your risk:
- Take it easy when starting new activities that can place stress on your ankles and feet. Start all new exercises gradually and increase the intensity and duration slowly, allowing your body to adjust to the added pressure and stress of these movements.
- Avoid hill running and exercise that places excessive stress on your tendons.
- Warm up. Always warm up first before any exercise. If you notice any pain during exercise stop, rest and contact your health professional.
- Wear appropriate footwear. Wearing shoes that are suited to the level of activity you are doing will provide the adequate cushioning and support for your feet. Replace old or worn out shoes. You may need arch supports if you are not feeling supported enough in your shoes.
- Do daily stretches. Take the time to stretch your whole body daily, including your Achilles tendon. This will help to maintain flexibility and could help avoid recurrent Achilles issues.
- Strapping and taping the Achilles tendon may be beneficial when doing exercise.
- Strengthen your calf muscles. The Achilles tendon can better handle stress when it has strong back up by the surrounding muscles.
- Allow adequate rest between activities.
- Cross-training high impact activities with low impact ones can strengthen the tendons and muscles. For example running and jumping to cycling and swimming.
Signs and Symptoms
Achilles Tendinopathy typically commences as a mild ache or burning pain at the back of the leg or above the heel. This can start at the beginning of an activity and worsen or come on suddenly during or after activity. If pain is severe and sudden and causes disability then the tendon may be ruptured and you should seek immediate medical attention.
Signs to watch out for:
- Mild to sever pain or tenderness in the Achilles tendons area
- Swelling or redness towards the lower leg
- Stiffness or loss of strength in the affected area
- Decreased movement in the ankle
- Feeling of sluggishness in the leg
There are 4 grades when it comes to Achilles tendinopathy according to the severity of the injury:
| Phase | Description | Prognosis | Healing time |
| 1 | Mild- pain after activity | Great – minimal treatment needed | Days |
| 2 | Moderate- Pain before and after activity. Pain gradually lessons during activity. | Good- minimal treatment, rehab program needed | Weeks |
| 3 | Severe- Pain with activity causing decrease in volume of activity. | Moderate- Rehab program needed | Months |
| 4 | Extreme- Pain during rest and activity. Worsening or progressing pain. | Severe- Intense rehab program or surgical intervention needed. | Years |
Treatment
Treatment of Achilles tendinopathy is dependent on the severity of the injury. Your physiotherapist is very skilled in treating these injuries and can assess, treat and monitor the injury. They will be able to provide you with appropriate exercise and advice that is suitable to the phase applicable to your injury. They are there to help fast track your recovery and get you back into your favourite activities.
Treatment can often consist of the following methods:
- Rest and recovery time
- Pain relief
- Stretching exercises
- Changes in sporting techniques
- Adequate footwear recommendations including orthotics
- Isometric exercises or low level training
- Avoiding certain exercises or activities
- Massage and soft tissue therapies
- Dry needling
- Stretching and foam rollers
- Referral to a specialist if surgery or cortisone injections may be warranted in extreme instances.
Rehabilitation and return to activity
Every injury is unique and every recovery program and duration is specific to your needs. Injuries to the Achilles tendon can take weeks or months to rest and repair. The use of crutches may be recommended to take some weight off the injury while it heals.
It is important to see a health professional for this rehabilitation program as it will be unique to your injury and will help get you back to your normal activities faster. Your physiotherapist will be able to monitor this healing and can discuss with you a suitable program with rehabilitation exercises and treatments that will gradually strengthen the tendon. These programs can include ultrasound, mobilisation techniques, stretching, sports massage, orthotics, dry needling or take home exercises.
If you are suffering from a complete rupture or tear of the Achilles tendon your physiotherapist may refer you to a specialist surgeon to have the tendon repaired surgically. Surgery is often followed by a plaster cast and an intense rehabilitation program followed by a strengthening program. These are supervised by your surgeon and your physiotherapist. Alternatively, you may follow a non-surgical approach, which has been shown to have just as effective long-term outcomes as surgery. Your surgeon and physiotherapist will be able to help you decide your treatment option based on your individual circumstances.
Returning to any activities should be gradual no matter what phase of injury and it is recommended that you follow your health professionals advice on when to recommence sporting activities so that you do not further injure the tendons.
If you or someone you know is suffering from an Achilles Tendon injury, call our friendly staff today or book an appointment online. Our trained Physiotherapists are here to keep you moving.

Always Consult a Trained Professional
The information above is general in nature and is only intended to provide a summary of the subject matter covered. It is not a substitute for medical advice and you should always consult a trained professional practising in the area of sports medicine in relation to any injury.
Acknowledgements
Images are courtesy of www.pexels.com
To find out how we can help please do not hesitate to contact our reception on (02) 6210 0060 or book an appointment.